 Wash your hands regularly and wear a face mask.
Learn more
Wash your hands regularly and wear a face mask.
Learn more
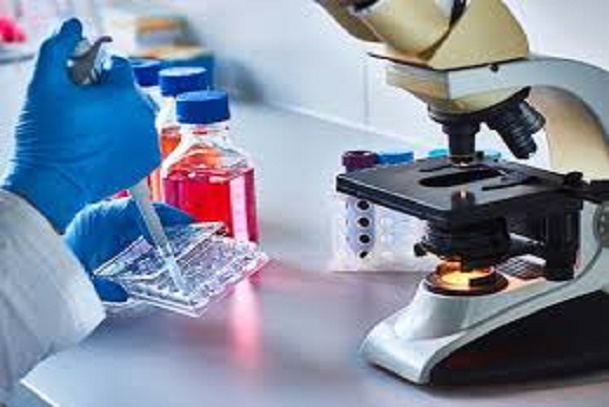
Diagnoses of Monkeypox
Diagnosing monkeypox among humans might be a little bit difficult due to its form or outlook i.e. resemblance with smallpox or chickenpox. In Nigeria, diagnosing monkeypox is usually by the patient’s history and the examination exercise that might show the pox lesions on the body.
However, monkeypox can only be diagnosed definitively in the laboratory where the virus can be identified by a number of different tests that need to be conducted in specialized laboratories using PCR (polymerase chain reaction), ELISA (enzyme-linked immunosorbent assay) or Western blotting tests (i.e. immunoblotting); although this diagnosis might rule out other possible and common diseases like smallpox.
For optimum diagnosis, specimens from lesions – vesicular swabs of lesion exudates or crusts stored in a dry, sterile tube (no viral transport media) and kept cold are usually used. Blood and serum can be used but often can be inconclusive because of short duration of viremia and timing of specimen collection. In order to interpret test results it is critical that patient information is provided with the specimens including: a) approximate date of onset of fever, b) date of onset of rash, c) date of specimen collection, d) current status of the individual (stage of rash), and e) age
Due to the unlikely outcome of diagnosis, most medical professionals are usually advised to be careful in dealing with patients who might have pox lesions showing all over their body while attending or treating them.
Also the clinical differential diagnoses that must be considered while attending to patients with monkeypox symptoms include other rash illnesses, such as, smallpox (even though it is eradicated), chickenpox, measles, bacterial skin infections, scabies, syphilis, and medication - associated allergies. Lymphadenopathy during the prodromal stage of illness can be a clinical feature to distinguish monkeypox from smallpox.
Treatment of Monkeypox
Currently there are no specific treatments or vaccines available for monkeypox infection, but outbreaks can be controlled. Vaccination against smallpox has been proven to be 85% effective in preventing monkeypox. Therefore it is recommended that:
Prevention of Monkeypox
Prevention for Individuals and Families
During human monkeypox outbreaks, close contact with other patients is the most significant risk factor for monkeypox virus infection. In the absence of specific treatment or vaccine, the only way to reduce infection in people is by raising awareness of the risk factors and educating people about the measures they can take to reduce exposure to the virus. Surveillance measures and rapid identification of new cases is critical for outbreak containment. These are number of other measures that can be taken to prevent infection with monkeypox virus:
Prevention for Medical Professionals
Also the government of each country could provide laws that restricts or ban the movement of small animals, mammals or rodents from one African country to another or across the continent. Captive animals that are potentially infected with monkeypox should be isolated from other animals and placed into immediate quarantine. Any animals that might have come into contact with an infected animal should be quarantined, handled with standard precautions and observed for monkeypox symptoms for 30 days.